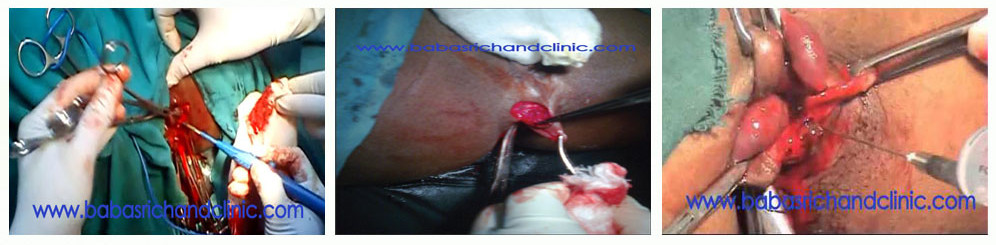
Hemorrhoidectomy:
Anal vascular cushions are present in everyone and are believed to contribute, in small part, to overall anal continence. The term hemorrhoids is used to refer to these cushions when they become enlarged and symptomatic.
These anal cushions are composed of plexuses of vessels within the anal canal that connect arterioles to veins without intervening capillaries. They are also normally supported by smooth muscle fibers (Treitz muscle) and connective tissues in the submucosa that help maintain their position in the upper half of the canal.
Repeated stretching of these attachments causes disruption and results in prolapse. Anatomically, these major vascular cushions are typically located in 3 main positions—left lateral, right anterolateral, and right posterolateral. When hemorrhoids are symptomatic, smaller, secondary cushions may be present between the main cushions.
Hemorrhoids present above the dentate line are classified as internal hemorrhoids. Hemorrhoids occurring below the dentate line are classified as external hemorrhoids.
External hemorrhoids are in sensitive anal canal skin and are painful, while internal hemorrhoids are in insensitive anal canal mucosa and are painless (unless complicated).
The anal canal is completely extraperitoneal. The length of the (surgical) anal canal is about 3-5 cm, with two thirds of this being above the dentate line and one third below the dentate line (anatomical anal canal).
Development of hemorrhoids:
Despite several years of study, the main etiology of hemorrhoidal disease is still largely unknown. Many proposed theories exist, but the most common, and perhaps most accurate, pertains to the abnormal sliding of the vascular cushions that is associated with straining and irregular bowel habits. Hard, bulky stools promote straining, which is more likely to push the cushions out of the anal canal. Furthermore, straining may cause engorgement of the cushions during defecation, making their displacement more likely. Congestion and hypertrophy of the anal cushions ensue, making them more prone to developing edema and bleeding.
Symptoms:
- Bleeding: Bleeding is the most common presenting symptom. It usually manifests as bright red blood, recognized first on the toilet paper with defecation and later becoming heavier and noticed in the toilet. With time, bleeding may be unrelated to defecation.
- Prolapse: Prolapse of internal hemorrhoids is highly characteristic of more advanced and chronic hemorrhoidal disease. The prolapsed internal hemorrhoids may reduce spontaneously or may need to be reduced manually. In rare cases, they may prolapse through the anal canal and become incarcerated.
- Pain/discomfort: In the absence of thrombosis or incarceration, hemorrhoids are usually painless. Dull pain after defecation is common with prolapsed hemorrhoids and is relieved by reducing the prolapse. If someone is experiencing severe pain, a complication of hemorrhoids or another diagnosis, such as anal fissure, abscess, or rectal ulceration, must be considered.
- Discharge/pruritus: Patients may experience mucoid anal discharge or fecal soilage as internal hemorrhoids prolapse through the anal canal. This irritation of the perianal skin can result in significant pruritus.
Complications:
Thrombosis and infection Thrombosis is the most painful complication of internal or external hemorrhoids. The pain is often severe enough to affect routine daily activities. While it can occur in large, prolapsed hemorrhoids, thrombosis is more common in external hemorrhoids. If the epithelium overlying the thrombosed hemorrhoid breaks down and allows invasion of bacteria, it may lead to infection, which is rare.
The incidence of hemorrhoidal bleeding that results in anemia is low.
Indication:
External hemorrhoids represent distended vascular tissue in the anal canal distal to the dentate line. Persons with thrombosed external hemorrhoids usually present with pain on standing, sitting or defecating. Acutely tender, thrombosed external hemorrhoids can be surgically removed if encountered within the first 72 hours after onset. Hemorrhoidectomy is performed through an elliptic incision over the site of thrombosis with removal of the entire diseased hemorrhoidal plexus in one piece. Caution must be exercised to avoid cutting into the muscle sphincter below the hemorrhoidal vessels. Infection after suture closure is rare secondary to the rich vascular network in the anal area. Stool softeners must be prescribed postoperatively to help prevent tearing at the suture line. Training and experience in general and skin surgery are necessary before the physician attempts this procedure unsupervised.
External hemorrhoids usually develop over time and may result from straining with stools, childbirth, lengthy car trips or prolonged sitting, constipation or diarrhea. External hemorrhoids represent distended vascular tissue in the anal canal distal (outside) to the dentate line (the junction between the rectal mucosa and the specialized skin of the anal canal, called the anoderm). External hemorrhoids are covered by anoderm and perianal skin richly innervated with somatic pain fibers. Diseases affecting the anal canal or the external hemorrhoidal vessels can be extremely painful.
External hemorrhoids often develop in healthy young persons and may suddenly become thrombosed. Persons with thrombosed external hemorrhoids usually present with pain on standing, sitting or defecating. The thrombosis is slowly absorbed by the body during the course of several weeks. A resolving thrombosis may erode through the skin and produce bleeding or drainage.
Acutely swollen and tender thrombosed external hemorrhoids can be surgically removed during the first 72 hours after onset. After 72 hours, the discomfort of the procedure often exceeds the relief provided by the surgery. Some patients still chose to undergo late surgery, although they should understand that without surgery the hemorrhoid will eventually become fibrosed and resolve over a period of days to weeks.
An elliptic incision can be made over the thrombosis, and the clot and the entire diseased hemorrhoidal plexus can be removed in one piece. Although the site can be left open, many physicians prefer to place subcutaneous sutures to limit postoperative pain and bleeding. Suturing in this area, historically, has been avoided because of fear of complications, yet the rich vascular network in the anal tissues usually provides for rapid healing.
Simple incision over a thrombus after the administration of local anesthesia can be performed to remove the clot, but this procedure has been associated with a significant rate of rethrombosis. Many experts now recommend excision of the entire thrombosis and the external hemorrhoidal vessels beneath. This procedure is more extensive than simple incision but usually yields a better outcome.